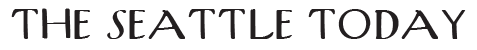Snohomish County health officials are encouraging residents to receive flu vaccinations before the Thanksgiving holiday following the county’s first flu death of the 2025-2026 season.
According to officials, a woman in her 60s with underlying health conditions died last Saturday.
Whilst flu deaths occur annually, the death serves as a reminder that respiratory viruses such as flu, COVID-19, and RSV can lead to severe illness, especially in young children, older adults, and those with existing health conditions, the health department stated.
During last year’s flu season, Snohomish County reported 53 flu-related deaths, the most in more than a decade.
The first flu-related death in last year’s flu season did not occur until January, prompting officials to remind everyone to stay current on vaccinations.
“It is a bit concerning to have our first death so early in the season. Things will only get worse,” stated Dr. James Lewis, Snohomish County Health Department Health Officer. However, it remains too early to determine how severe the season could become.
“It’s a good idea to get vaccinated at least one to two weeks before a family gathering. This gives your body enough time to build up immunity and offer protection,” Lewis stated.
Officials recommend anyone who is sick should stay home, cover coughs and sneezes, and wash hands thoroughly.
The early timing of Snohomish County’s first flu death, occurring in mid-November compared to January during the previous season, raises concerns amongst public health officials about the potential trajectory of the 2025-2026 influenza season. Early-season deaths can signal either particularly virulent circulating strains or widespread transmission beginning earlier than typical seasonal patterns.
The victim’s age, in her 60s, and presence of underlying health conditions align with well-established risk factors for severe influenza outcomes. Individuals aged 65 and older experience higher rates of flu-related complications, hospitalisations, and deaths compared to younger, healthier populations due to age-related immune system decline and higher prevalence of chronic conditions that increase vulnerability.
The 53 flu-related deaths Snohomish County reported during the previous season, described as the most in more than a decade, indicates the 2024-2025 flu season was unusually severe for the region. This elevated mortality creates context for heightened concern about the current season, as consecutive severe seasons can strain healthcare resources and fatigue public compliance with preventive measures.
Dr. Lewis’s statement that “things will only get worse” reflects epidemiological understanding that flu activity typically intensifies from autumn through winter, peaking between December and February in the Northern Hemisphere. The early death suggests transmission is already established in the community, with potential for amplification as holiday gatherings, indoor crowding, and seasonal factors facilitate viral spread.
The recommendation to vaccinate one to two weeks before family gatherings reflects the immunological timeline required for vaccine-induced protection to develop. Following vaccination, the immune system requires approximately two weeks to produce sufficient antibodies conferring protection against influenza strains included in the vaccine formulation.
The Thanksgiving holiday, occurring in late November, creates particular transmission risks as extended family members from different households and geographic areas gather indoors for prolonged periods, facilitating respiratory virus spread. Indoor gatherings during cold weather, when ventilation is reduced and people remain in close proximity, create optimal conditions for influenza transmission.
The health department’s reminder about the convergence of multiple respiratory viruses, including flu, COVID-19, and RSV, reflects the reality that these pathogens circulate simultaneously during autumn and winter months, creating compounded risks for vulnerable populations. The concurrent circulation complicates diagnosis, as symptoms overlap substantially, and increases overall burden on healthcare systems managing multiple respiratory illness surges.